Editorial: Is there a role for pure clinical prediction models in prostate cancer in the contemporary era?
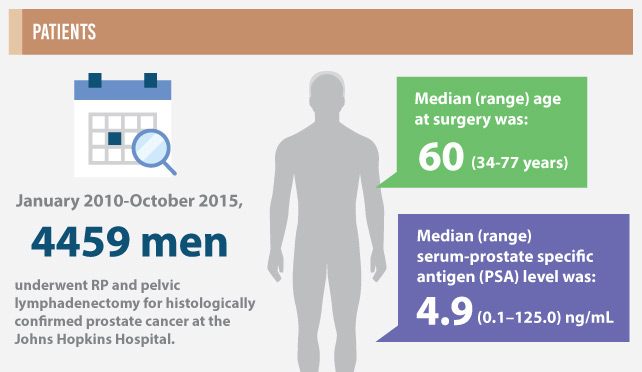
The identification of men with localised prostate cancer at higher risk of adverse pathological outcomes after radical prostatectomy (RP) would assist physicians in preoperative patient counselling and in tailoring the most appropriate treatment strategy. In this issue of the BJUI, Tosoian et al. [1] have updated the Partin Tables in contemporary patients with localised prostate cancer. The authors should be commended for undertaking a well-performed study evaluating a large cohort of patients treated at a high-volume centre. Notably, they were able to show that the Partin Tables still represent an accurate tool for identifying men at higher risk of adverse pathological features [1]. Having said this, the first question we should ask ourselves is whether preoperative models based on clinical variables only still play a role in contemporary patients. The Partin Tables were developed in 1993 and since then they have undergone a series of updates, all of which are based on virtually the same variables included in the original analyses [1]. However, recent implementations, including biomarkers and imaging, have been introduced to better stage prostate cancer. These novel approaches are usually added to clinical variables to improve patient risk stratification. Multi-parametric MRI (mp-MRI) represents the major game changer in this setting, being now recommended for prostate cancer staging in all men with high-risk disease and in those with less favourable intermediate-risk prostate cancer [2]. In the era of modern and sophisticated approaches, are models using clinical variables only still clinically valuable? To answer this question, we can consider two major settings, namely nodal and local staging.
When assessing the risk of lymph node invasion (LNI) at diagnosis, mp-MRI and positron emission tomography/CT scan are characterised by a low sensitivity and, therefore, are not recommended for the identification of patients who should receive a lymph node dissection (LND) [2, 3]. Conversely, the updated Partin Tables depicted a remarkably high accuracy (>90%) in predicting LNI. This supports what is currently recommended by virtually all guidelines, which indicate that candidates for extended LND (eLND) should still be identified according to a combination of clinical variables only. However, although the Partin Tables might assist clinicians in identifying patients more likely to harbour LNI, the lack of the uniform adoption of an eLND template might have resulted in a substantial under-estimation of the real LNI risk [4]. Other tools specifically developed to predict LNI among men treated with eLND could better assist clinicians in identifying men who should receive an eLND [2, 5].
Similarly, when considering local staging, mp-MRI is characterised by a high specificity but a relatively low sensitivity in detecting small, microscopic foci of extracapsular extension and seminal vesicle invasion (SVI) [6]. Conversely, the updated Partin Tables depicted a predictive accuracy of >80% in predicting SVI, despite the lack of individualised data on the extent and volume of extraprostatic extension. For all these reasons, clinical risk models still represent the cornerstone for the identification of men at higher risk of adverse pathological findings. Additional data coming from sophisticated imaging modalities may further improve individualised risk predictions [6] and better assist clinicians in tailoring the most appropriate treatment approach. However, imaging and biomarkers should complement, rather than substitute, currently available clinical risk models.
In conclusion, preoperative predictive tools based on clinical parameters still play an important role in the management of patients with clinically localised prostate cancer. Any staging model including additional approaches, such as imaging and/or biomarkers, is welcomed only when it is shown to improve prostate cancer staging in terms of both accuracy and cost-effectiveness.
How to Cite
Gandaglia, G., Fossati, N., Dell’Oglio, P., Montorsi, F. and Briganti, A. (2017), Is there a role for pure clinical prediction models in prostate cancer in the contemporary era?. BJU International, 119: 652–653. doi: 10.1111/bju.13833