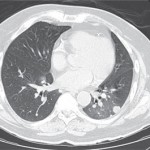
Editorial: mTOR-related non-infectious pneumonitis: a potential biomarker of clinical benefit?
The study by Atkinson et al. [1] published in the present issue of the BJUI is the largest study to date to address the role of non-infectious pneumonitis (NIP) as a predictive biomarker in patients with RCC who are treated with mammalian target of rapamycin (mTOR) inhibitors. It is also the first article to correlate mTOR-related NIP with improved overall survival (OS). Until now, only radiological response as measured by RECIST and progression-free survival (PFS) had been correlated to the onset of NIP in two small retrospective studies [2, 3], but the results obtained in those studies were contradictory and, therefore, this correlation remains controversial.
While the predictive relationship between NIP and OS needs to be further investigated in well-designed prospective clinical trials, the implications of such a relationship may be significant because no predictive biomarkers for mTOR inhibitors have been validated to date. In the era of targeted therapies, the detection of biomarkers of treatment efficacy is crucial to differentiate the subpopulations of patients who are most likely to benefit from treatment. Several biomarkers, such as the development of arterial hypertension and hypothyroidism, have been correlated with improved outcomes in patients with advanced RCC treated with vascular endothelial growth factor pathway inhibitors [1]; however, there are currently very limited data regarding the potential predictors of the clinical efficacy of mTOR inhibitors. A recent study by Lee et al. [4] showed that greater increases in serum cholesterol levels from baseline in patients with advanced RCC treated with temsirolimus were significantly associated with longer PFS and OS. Interestingly, temsirolimus-related hypertriglyceridemia and hyperglycaemia were not associated with improved clinical outcomes. Although NIP or hypercholesterolaemia must still be validated prospectively to ascertain whether they are true surrogate biomarkers of pharmacodynamic effect or just confounding epiphenomena, these promising findings may be the first steps in the identification of predictive biomarkers in mTOR inhibitor therapy.
Other important aspects addressed by Atkinson et al. [1] are the uncertainty of the pathogenesis of mTOR-related NIP and the lack of clinical predictive factors. Older age and treatment with everolimus were the only significant predictive factors of onset of NIP in their multivariate analysis. Similarly, a retrospective study by Dabydeen et al. [2] showed a statistically nonsignificant higher incidence of NIP in patients with RCC treated with everolimus compared to those treated with temsirolimus. Interestingly, in a randomized phase II study testing three different dose levels of temsirolimus (25,75 and 250 mg/week) in patients with advanced RCC, none of the six patients diagnosed with NIP were in the highest dose group of 250 mg/week [5], suggesting that mTOR-related NIP might have a non-dose-dependent pathogenesis. Similarly, a meta-analysis of 2233 patients affected by different tumours including RCC treated with an mTOR inhibitor failed to show any relationship between median treatment duration and incidence of NIP [6]. Finally, underlying respiratory conditions before treatment, such as the presence of lung metastases [6], chronic obstructive pulmonary disease or smoking habit [2], were not shown to be predictive factors of development of mTOR-related NIP. Another study by White et al. [3] showed that the development of pneumonitis in patients with RCC treated with everolimus was not associated with more impaired baseline pulmonary function tests, indicating that pulmonary function tests may not help identify patients with an increased risk of pneumonitis nor predict its severity. At present, there are therefore very few pretreatment clinical predictive factors to help clinicians identify patients at higher risk of developing mTOR-related NIP.
In conclusion, given the potential value of NIP as a predictive biomarker of survival in patients with RCC treated with mTOR inhibitors, Atkinson et al. [1] suggest that efforts should be made to avoid dose reductions and treatment discontinuation whenever possible. However, predictive factors of the severity of lung toxicity are needed to identify those patients at risk of developing life-threatening NIP as the maintenance of dose intensity may be crucial for maximizing clinical benefit.
Alejo Rodriguez-Vida, Noan-Minh Chau and Simon Chowdhury
Department of Medical Oncology, Guy’s Hospital, London, UK
References
- Atkinson BJ, Pharm D, Cauley DH et al. mTOR inhibitor-associated non-infectious pneumonitis in patients with renal cell cancer: management, predictors, and outcomes. BJU Int 2014; 113: 376–382
- Dabydeen DA, Jagannathan JP, Ramaiya N et al. Pneumonitis associated with mTOR inhibitors therapy in patients with metastatic renal cell carcinoma: incidence, radiographic findings and correlation with clinical outcome. Eur J Cancer 2012; 48:1519–1524
- White DA, Camus P, Endo M et al. Noninfectious pneumonitis after everolimus therapy for advanced renal cell carcinoma. Am J Respir Crit Care Med 2010; 182: 396–403
- Lee CK, Marschner IC, Simes RJ et al. Increase in cholesterol predicts survival advantage in renal cell carcinoma patients treated with temsirolimus. Clin Cancer Res 2012; 18: 3188–3196
- Atkins MB, Hidalgo M, Stadler WM et al. Randomized phase II study of multiple dose levels of CCI-779, a novel mammalian target of rapamycin kinase inhibitor, in patients with advanced refractory renal cell carcinoma. J Clin Oncol 2004; 22: 909–918
- Iacovelli R, Palazzo A, Mezi S, Morano F, Naso G, Cortesi E. Incidence and risk of pulmonary toxicity in patients treated with mTOR inhibitors for malignancy. A meta-analysis of published trials. Acta Oncol 2012; 51: 873–879