Editorial: ‘Killing Two Birds With One Stone’ – PROMS from the ProtecT Trial
Very few areas of medicine generate more controversy than the management of clinically localised prostate cancer. This is in large part due to the somewhat conflicting nature of the scant level I evidence that exists on the subject. Whereas the Scandinavian Prostate Cancer Group Study Number 4 (SPCG-4) demonstrated a clinically meaningful and durable survival advantage for surgery when compared to watchful waiting in a predominantly White Scandinavian population of patients with clinically palpable yet localised prostate cancer [1], the Radical Prostatectomy Versus Observation for Localized Prostate Cancer (PIVOT) trial reported a mostly null effect of surgery in a predominantly older, less healthy population of American patients with clinically indolent disease [2]. Neither trial addresses the effect of radiotherapy on prostate cancer survival and both may lack relevance in contemporary prostate cancer practice.
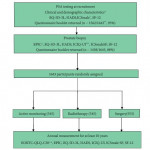
For these reasons and a myriad of others, the medical community eagerly awaits the results of the Prostate Testing for Cancer and Treatment (ProtecT) trial [3]. With a fastidiously designed protocol that involves 337 primary care centres across nine cities in the UK, the use of dedicated study nurses, the successful enrolment of pre-specified sample size targets, and the inclusion of patient-reported quality-of-life measures, the ProtecT trial is poised to make enormous inroads for men with prostate cancer and the providers who care for them.
In this issue of the BJUI, the investigators from the ProtecT trial publish baseline patient-reported outcome measures (PROMs) from the ProtecT trial [4]. While others have previously reported baseline PROMs in large comparative effectiveness studies [5], the findings from this study are notable for several reasons. First, this is the first randomised trial comparing the effect of surgery, radiation, and active monitoring on PROMs. While several high-quality prospective observational cohort studies have reported long-term quality-of-life outcomes after prostate cancer treatment [6, 7], ProtecT will offer randomised comparisons that minimise confounding and selection bias from the outset. Second, the ProtecT trial will not only measure disease-specific health-related quality of life through the use of psychometrically validated survey instruments, such as the Expanded Prostate Index Composite, but also general health-related quality of life through the use of the European Organisation for Research and Treatment of Cancer (EORTC) Quality of Life Questionnaire (QLQ) C-30 (as well as depression and anxiety through the use of the Hospital Anxiety and Depression Scale). Finally, and perhaps most importantly, the investigators collected baseline PROMs at the time of the first biopsy before cancer diagnosis, which will offer distinct advantages when modelling patient-reported function over time, as well as avoiding recall bias associated with retrospective collection of baseline patient-reported outcomes.
In the absence of the long-term survival data from randomised trials comparing surgery and radiation, previous studies have rightly focused on understanding how the effect of prostate cancer treatments differ with respect to PROMs. With the ProtecT trial, we will not only start to have answers to longstanding questions about how surgery, radiation and active surveillance compare with respect to clinical outcomes, such as survival and cancer control, but also with respect to PROMs. By addressing both of these domains, the ProtecT investigators are in position to ‘kill two birds with one stone’ and in so doing will undoubtedly make large strides in facilitating data-driven decision-making for patients with prostate cancer worldwide.